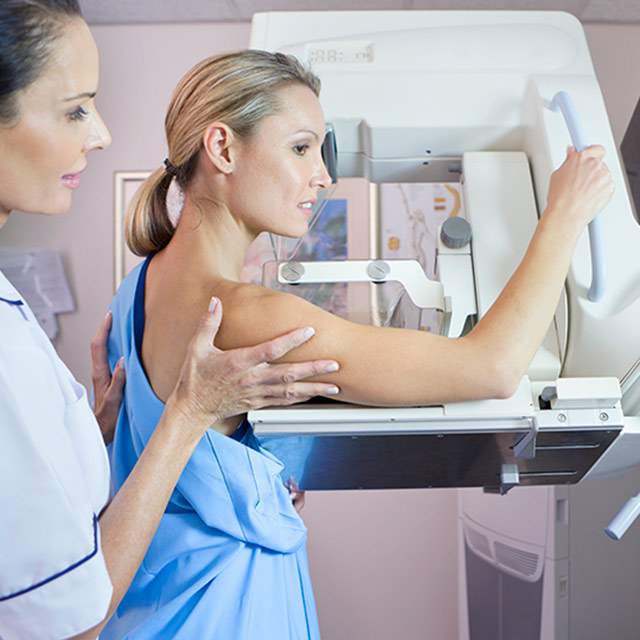
Medical guidelines may change. What to know about your own breast cancer risk.
Many women are familiar with the conventional wisdom that they should start getting mammograms every year, starting at age 50.
For many years, that was common advice for women at average risk of developing breast cancer. (Women with a higher-than-normal chance of having breast cancer have been urged to start getting mammograms before age 50. We’ll get to risk factors later in this article.)
The official medical guidance on mammograms may change soon, however. An influential national health care organization is proposing new recommendations: that women with average breast-cancer risk start getting mammograms at age 40, and repeat them every other year instead of annually.
The U.S. Preventive Services Task Force is the national organization considering this change. This group makes recommendations to the medical community about different screening tests for various diseases.
Mammograms are X-ray images of the breasts. Their purpose is to detect cancerous tumors in the breast when they are small enough to be treated easily. Earlier treatment is easier for women to manage than more intense treatment of cancer that has spread. Earlier treatment is also more likely to save someone’s life than more complicated treatment after the cancer has spread to other parts of the body.
Dr. Kelly Hewitt, a breast surgeon at the Vanderbilt Breast Center, explained the thinking behind the possible change in recommendations.
She acknowledged that there are several medical organizations that offer slightly different recommendations about when women should start getting mammograms, ranging from age 40 to 50 for those at average risk for this cancer.
“The important thing about the U.S. Preventive Services Task Force is that it’s very highly regarded, and a lot of insurance companies take their cue from them,” Hewitt said. Medicare and major insurance companies are likely to decide what mammograms they will pay for based on what the task force decides.
Lowering the age for first mammograms to 40 “is a great step,” Hewitt said. “I think that women should be getting mammograms at age 40 and that is, again, women who are at average risk. What has prompted a lot of this is that we’re seeing an increased incidence in breast cancer in women who are under age 50. And so, by extending screening mammograms to younger ages, the idea is that you’ll find these cancers early and be able to treat them before they progress.”
What the numbers say
In 2000, about 115 out of 100,000 women in the U.S. under age 50 were diagnosed with breast cancer. By 2019, that rate had risen to 137 diagnoses out of 100,000 women. That’s not a huge change but it’s steadily rising, Hewitt said. The possible new guidelines are meant to catch those younger cases early.
Finding breast cancer early potentially saves tens of thousands of lives every year. Consider some numbers:
- About one in eight American women will have breast cancer at some point.
- It’s the most common cancer diagnosis for women.
- Medical experts predict that almost 300,000 American women will be diagnosed with breast cancer in 2023.
- Breast cancer is the number-two cause of cancer-related deaths among U.S. women, second only to lung cancer.
- About 40,000 American women die of breast cancer every year.
Know your own risk for breast cancer
Whether the official task force guidelines change or not, women should talk to their doctors about their own individual chances of developing breast cancer. It will be different for different people, but factors that increase the risk of having it are:
- Age: Risk increases as you get older.
- Certain gene mutations: The most well known affect the BRCA1 and BRCA2 genes.
- A family history of breast cancer: This is true especially if the relative with breast cancer is a close relative or was young when diagnosed.
- Previous diagnosis: If you have had breast cancer in the past, that increases risk.
- Dense breasts: Having dense breast tissue increases risk.
- Estrogen exposure: Over your lifetime, breast cancer risk rises with greater use of estrogen therapy.
Don’t worry, most mammograms show no cancer
Mammograms are uncomfortable, but women who feel reluctant to get this screening done because they’re afraid of the findings should take comfort: Most mammograms show no problems.
“The vast majority of mammograms aren’t going to find cancer,” Hewitt said. “About 8% to 10% of women who have a mammogram then go on to have additional imaging, or need a biopsy. And even of those women who need a biopsy, 80% are benign. So, you know, it most likely it’s not going to be anything.”
False positive readings (when the mammogram says there is cancer, when there really isn’t) happen fairly frequently, however. Getting a mammogram every other year, as the proposed new guidelines suggest, instead of every year, may cut down on the number of false positive results.
Anyone with questions about their personal risks for breast cancer should ask their doctors about what mammogram schedule, if any, is appropriate for them.

Help for women at high risk for breast cancer
Vanderbilt has two clinics specifically designed to manage and support people who are at high risk for breast cancer:
Vanderbilt Health One Hundred Oaks
719 Thompson Lane, Suite 25000
Nashville, TN 37204
Vanderbilt Breast Center
324B Cool Springs Boulevard
Franklin, TN 37067
For appointments, call (615) 322-2064.